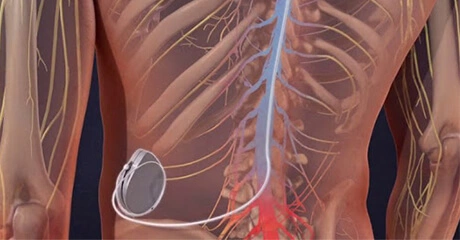
Epidural Steroid Injections
- Quick Links: > More About IPI
- > Procedures
- > Diagnosis
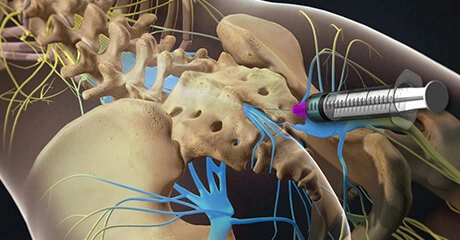
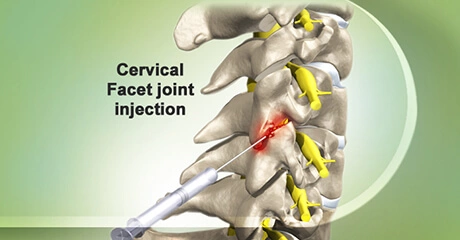
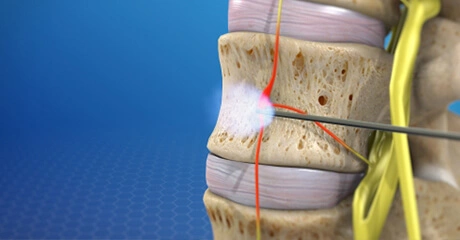
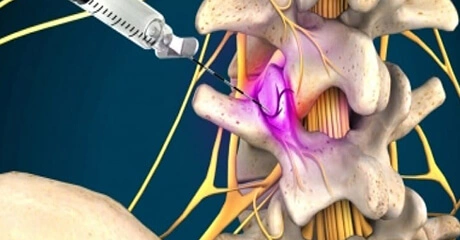
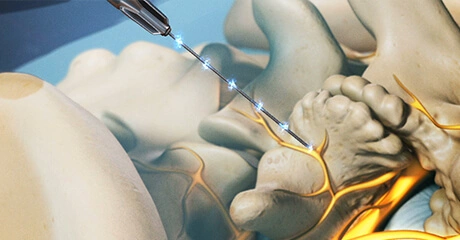
This injection procedure is performed to treat the pain of an inflamed nerve in your spine. If you have a herniated disc, spinal stenosis, or some other problem that is pressing on a nerve, it may help you. Steroid medication can reduce the swelling and inflammation caused by spinal conditions. The steroid medication is injected into the epidural space, which is the space around the inflamed nerve. It bathes the painful nerve and relieves pain and swelling. In some cases, it may be necessary to repeat the procedure as many as three times to get the full benefit of the medication. Many patients get significant relief from only one or two injections.
- 36
- 125